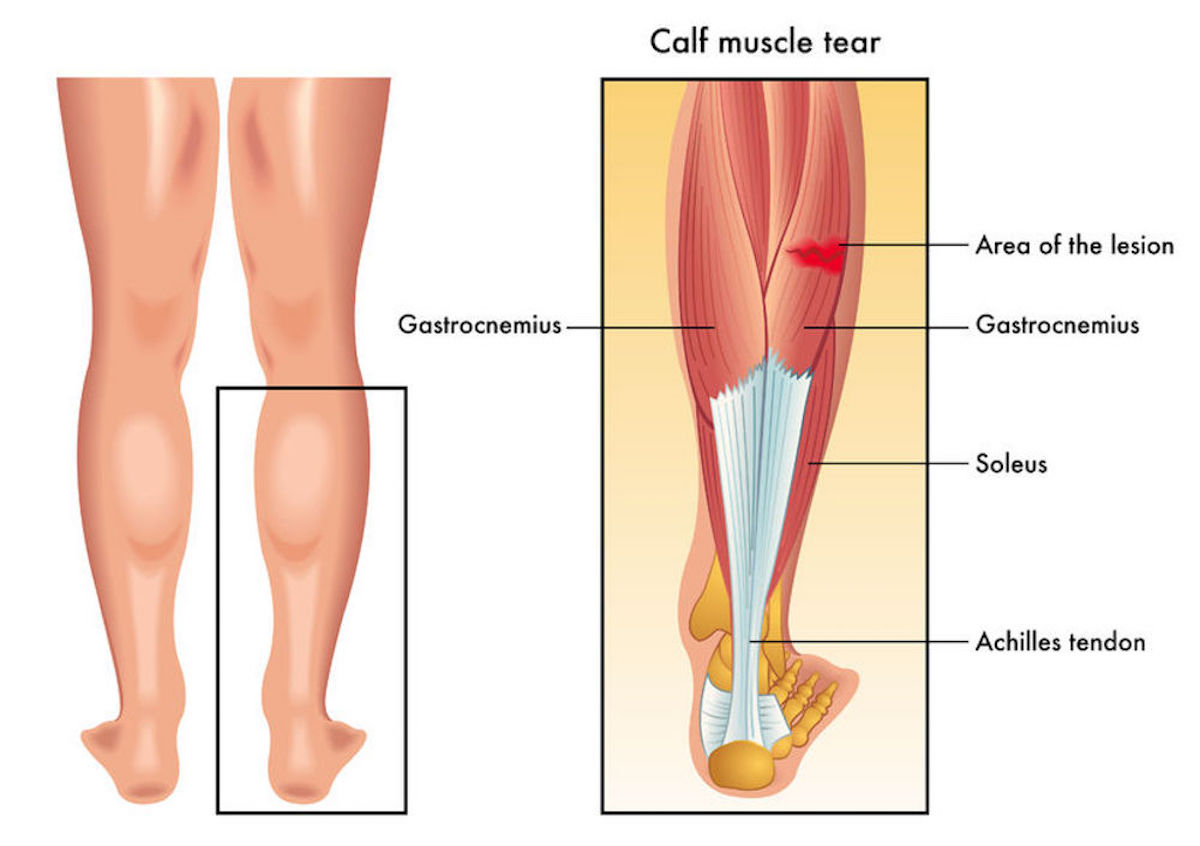
The calf complex is a powerhouse in the legs, and consists of two main muscles, gastrocnemius which lies more towards the surface and soleus, which sits underneath the gastrocnemius. Pain in this region can be due to a muscle strain, muscle cramping, referred pain from higher up such as the nerves in your leg or lower back as well as medical sources such as a deep vein thrombosis.
Common types of calf injuries and calf pain:
Calf strains
Calf pain is typically just below the knee and above the achilles tendon. Calf strains are the most common type of calf pain and can occur in the gastrocnemius muscle, soleus and plantaris muscles. Although less common, they can occur in other lower limb muscles.
The most common area of a calf strain is in the medial head of the gastrocnemius 58-65%, lateral head 8%-38% and soleus 58%-66% (Counsel 2015). In elite AFL players, soleus calf strains were evident in up to 84% of all calf strains (Green et al. 2020).
Calf strains usually occur after an explosive effort such as sprinting, changing direction or can even occur over time where a build up of tightness and discomfort continues to worsen until you have to cease activity. Calf strains can happen at any age, but male masters running athletes (>35 yo) have the highest prevalence of calf strains (Taunton 2002).
This is generally caused by a reduction in calf capacity (strength & endurance) and training load errors such as large increases in volume (more kilometres) or intensity (more speed) being the biggest factors.
Referred calf pain
Less common types of calf pain can be referred pain to the lower leg from the lumbar spine or gluteal muscles. This can present as an episode of sharp sudden pain or gradual onset with a similar feeling to a calf strain such as a tightening, cramp sensation or discomfort.
Lumbar referred calf pain is typically variable and more spread out in its location and tends not to be localised to one area. Referred pain can be ruled out by neurodynamic testing (these essentially wind up your nerves to see if it reproduces your pain) performed by your physiotherapist.
Cramp
The most typical type of cramp would be an exercise associated muscle cramp (EAMC) which can happen either during or post exercise. Cramps can occur for many reasons (e.g. low electrolytes) but in an exercise setting, they tend to occur in less conditioned individuals, or those which have high training loads who push their muscles to fatigue on a regular basis.
Regardless, cramps are commonly caused by fatigue or poor muscle endurance / capacity and electrolyte loss. Cramps are typically not serious and can be eased with light stretching and soft tissue work. Most importantly, ensuring the capacity of your calf muscles can tolerate your level of exercise is an important consideration.
Calf Overload Syndrome
Calf overload syndrome is the combination of increased training loads above and beyond the tolerance of your calf and muscle fatigue. This causes a rapid tissue overload within the calf musculature resulting in pain & discomfort.
Usually the pain slowly builds up with running and should be resolved when running ceases. The biggest risk factors for this type of calf pain is typically related to large changes in load (i.e. speed or distance) or running technique (changing stride length or forefoot / heel striking).
Additionally, a lack of rest in between training periods and poor capacity of the gastrocnemius and soleus muscles are risk factors for this condition. As discussed later on, the capacity of the calf musculature plays an important role in calf muscle injury reduction.
Less common calf pain
Whilst not as common as other types of calf pain may include contusions such as a hit on the lower limb during sport, Bakers cyst and even deep-vein thrombosis following surgery or long flights.
How do I know if I strained my calf?
Depending on severity of injury, most will report a sensation of tightening or discomfort during or post activity. In more severe cases of a muscle tear, some report the sensation that somebody has hit or shot them in the back of the leg alongside a ‘popping’ noise. This may cause severe pain accompanied with difficulty walking.
Calf strain symptoms include:
- Local Tenderness to touch at point of discomfort
- Bruising
- Pain on calf stretch
- Pain with activity
- Swelling
The differences between a Gastrocnemius strain and soleus will generally differ from location and intensity of discomfort. For example, a soleus strains are generally less severe with some being able to walk around relatively comfortably.
Soleus strains generally are a little bit lower (towards the middle) inner part of your lower leg. In contrast, a gastrocnemius strain will generally vary from mild to severe pain and you may have difficulty in walking initially. These will generally be localised to the upper calf on either side.
Risk factors for calf pain
- Older age
- Poor load management (e.g. doing too much too soon)
- Calf capacity / strength / endurance
- Change of Terrain (e.g. incorporating more hill work or trail running from road running as this can put more demand of the calf musculature)
Alongside load management, calf endurance and strength play a vital role in injury prevention.
For example, during running, the calf muscles can take up to 6 – 8 x your body weight in force.
Therefore, if you had reduced strength or endurance, thus lower capacity your risk of a calf injury may be higher. So how do you know if your calves are lacking in this area?
Below is a table with normal values that represent good calf endurance for your age:
Single Leg Calf raise norms 2s up 2s down
- 20’s: male (M) 38, female (F) 31
- 30’s: male (M) 33, female (F) 28
- 40’s: male (M) 29, female (F) 25
- 50’s: male (M) 24, female (F) 23
- 60’s: male (M) 20, female (F) 20
- 70’s: male (M) 15, female (F) 17
- 80’s: male (M) 10, female (F) 15
Exercises to target your calf
It is important that you target both your gastrocnemius and soleus muscles to strengthen your calf completely. These will range from your basic strengthening exercise to more higher level plyometric (jumping / hopping) exercises.
Below are some exercises that target both the gastrocnemius and soleus:
- Double leg calf raise (off a step) +/- weight
- Single leg calf raise (off a step) +/- weight
- Bent knee Double / Single calf raise (off a step) +/- weight
- Creepers / Toe walking with weight +/- weight
- Pogo & hopping variations (Double leg & single leg)
- Jumping (i.e. box jumps, broad jumps, vertical jumps)
These are an non-negotiable when it comes to treatment for a pulled calf muscle.
How do you relieve severe calf pain?
If you’ve just suffered a calf strain or find yourself with severe calf pain, follow the “PEACE & LOVE” acronym rather than the more simplistic “RICE”.
- Protection – unload & restrict movement for 1 – 3 days after injury
- Elevate – place foot higher than the heart as often as possible
- Avoid anti-inflammatories – this can have negative effects on long term healing! Inflammation is a normal part of the healing process.
- Compression – Use tape or compression bands to limit swelling & tissue bleeding
- Education – Talk to your physiotherapist and get the right information & advice about your injury.
- Loading – Resume appropriate loading of the injured tissue as soon as tolerated
- Optimism – Stay realistic but optimistic that things will improve. Negative thoughts towards your injury can slow the process down.
- Vascularisation – Pain free cardiovascular exercise such as bike riding can help increase blood flow to local tissue.
- Exercise – Restore mobility, strength and proprioception by adopting an active approach to recovery
Physiotherapy for calf muscle pain
The first point of call for physiotherapy for calf pain will be to determine mechanism of injury, severity of injury and most importantly what exactly causes your calf pain. A physiotherapist should also seek to rule out other uncommon but potentially nasty causes (e.g. deep vein thrombosis).
A Physiotherapist will
- Assess your calf range of motion
- Perform physical tests to rule out other potential causes
- Test your functional capacity (e.g. hopping, jumping or jogging if applicable)
- Test your calf capacity
After a detailed assessment, you and your physio in collaboration will determine a treatment plan on day 1 to get you back to your desired activities in the shortest time frame possible.
Depending on severity, early calf tear treatment may include soft tissue work such as massage to help manage your pain and progress towards loading the calf muscles as soon as tolerated. This may start with basic double leg & single leg calf raises, and progressing to plyometrics (jumping & hopping) and a return to sport/activity program individually tailored to you.
Stretches for preventing calf pain
Whilst popular, stretching has not been found to reduce risk of any injury including the calf (Small et al. 2008). However, stretching generally isn’t harmful so if it is something you find beneficial then it’s safe to continue.
So what is the best for preventing calf pain?
Building strength & endurance to build capacity is key to rehabilitation and minimising recurring calf strains and injuries in runners generally. No amount of stretching or massage will help build calf capacity thus should not be the focus of a robust rehab program.
Alongside this, load management is vitally important to reducing your calf injury risk. That is, avoiding large spikes in training (e.g. dramatically increasing your distance or speed) will help to minimise calf re-injury.
A safe amount for most people to increase their training load is 5-10% per week. Of course this is only a guide, and where possible individualized advice on your specific set of circumstances is preferred.
How long should you rest a strained calf muscle?
Generally we would aim to rest for no more than 1 – 3 days depending on severity. The key to regaining function is movement. Prolonged rest is generally unhelpful, as it can lead to further deconditioning of not only the calf, but the other muscles in your leg. This can lead to a longer rehabilitation period, delayed return to your chosen recreational activity and increased risk of re-injury.
What next?
If you’d like to chat to one of our expert physios, please don’t hesitate call us on 8490 0777 email us at [email protected]
If you’re ready to start your journey to improved calf function and reduced pain, you can book online here.

