Lower back pain is extremely common, so common in fact that up to 90% of people will experience it in their lifetime. Whilst lower back pain can be anxiety-provoking and very painful, most will recover reasonably quickly from an acute onset of lower back pain.
Recovery from an episode of back pain usually occurs within 2-6 weeks, with initial symptoms beginning to decrease within the first 2 weeks or even a few days.
When a lower back irritation or injury occurs, it can either be a sudden event, such as lifting something unexpectedly heavy or even as seemingly simple as putting on your shoes in the morning. It may also be more gradual, for example waking up in the morning with some mild discomfort only for it to get progressively worse as the day goes on.
This doesn’t mean your core or back is weak, usually there is a combination of things that contribute over time that lead to lower back problems – we will discuss in more detail later on!
Why is lower back pain so painful
The initial onset of acute pain in your lower back can be related to the activation and sensitisation of local nerves by ‘possible’ tissue injury or irritation to the muscles, ligaments, discs, joints or even nerves within the lower back. Lower back pain can also coincide with sciatica-type symptoms such as referred pain or pins and needles into the buttocks or legs, muscle spasms and decreased mobility and movement.
Any form of injury to the body will lead to an inflammatory response, which can result in a further increase in sensitivity of the local nerves resulting in a greater discomfort, pain and movement restriction. Whilst this can cause mild, moderate and even severe pain, the inflammatory response is a normal part of the healing process and tends to reduce within 3-10 days.
Pain is very complex and your brain is hardwired to keep you safe! We’ll discuss more about pain and pain management later but it’s important to know that severity of pain does not always match the severity of injury. This just means that our pain system might be overprotective at times, and overdo pain how much pain you experience.
That being said, if you are experiencing any of the following, contact your GP or physiotherapist as soon as possible:
- Numbness / pins and needles in saddle region
- Unrelenting night pain
- Altered bladder or bowel function
- Unexplained weight loss
These symptoms can signify that something more serious or sinister is at play. An experienced physiotherapist will ask you about these amongst other things and ensure that you are SAFE to move within your limits in the early stages.
As previously mentioned, there are a variety of things that can contribute to back pain. Consider the following scenario:
You’ve noticed some discomfort in your lower back for a couple of weeks but nothing that you’ve put much thought to. Then one day you go to put your shoes on whilst sitting down and you feel a sudden pain and muscles spasms in your lower back
Naturally, most people in this scenario tend to blame this simple action of putting on their shoes as the cause of their back pain, but there is almost always more to the story than this.
There are a multitude of factors that can contribute to the onset of lower back pain including:
- A sharp increase in activity in previous days or weeks
- Older age
- Lack of sleep
- Previous injury
- Psychological factors including increased stress, anxiety, depression
It is rarely one movement in a given moment or poor posture that is to blame for the onset of lower back pain, but a combination of the aforementioned factors. One of the most common being performing an unaccustomed activity (e.g. for example repeated bending and lifting when moving house), causing your back to be exposed to loads greater than it can cope with over this period of time, which causes an irritation to the structures in the lower back.
Chronic back pain – Why is it so painful?
Chronic pain essentially means pain that has persisted for longer than 3 months. As we discussed earlier, there is a combination of factors that contribute to people having persistent lower back pain.
Your brain is designed to protect you and keep you safe, and it generally does a very good job at this. Our past experience helps guide how we act, and this is no different with pain. In chronic pain, you can think about your brain as an over sensitive alarm system that wants to warn you about anything that might be potentially dangerous. This is essentially why chronic back pain is so painful, which we will explain in more detail below.
It collects a massive amount of information from your surroundings, your past experience and determines whether a given situation is safe or potentially dangerous. In each situation, the brain weighs up the information – is there evidence that this situation is more likely to be dangerous or safe? If your brain determines that it’s dangerous, it will more likely respond with pain. This pain serves as a warning system to the rest of your body to get out of that situation.
Due to these recent advances in pain science, we know that tissue damage is poorly correlated to symptoms of severity in chronic pain. This idea can be challenging to wrap your head around, as we have spent our whole lives with the notion that tissue damage = pain. For example, have you ever stepped on a block of lego unexpectedly? It really hurts! But rarely is there tissue damage.
This does not mean that there is no contribution from our tissues (joints, muscle, etc) but rather is only a part of the puzzle.
The following factors all contribute to how much pain you experience:
- Psychological factors (fear of movement, stress, depression, catastrophizing and thinking you won’t ever get better),
- health (poor general health, low energy and comorbidities),
- lifestyle (poor sleep, overweight, smoking and living a sedentary lifestyle) or
- social (relationships, issues at work or home, financial difficulties, job and stressful life events)
- Your previous experience with pain (e.g. if you performed a movement that caused it)
We highly recommend watching the following two videos for added clarity around chronic pain.
What helps when your lower back hurts
Alongside some education and advice on what is happening in your lower back, movement is essential to reducing pain! Our spines are designed to move, so in the early stages, performing some movements that are comfortable and don’t increase your pain are usually helpful.
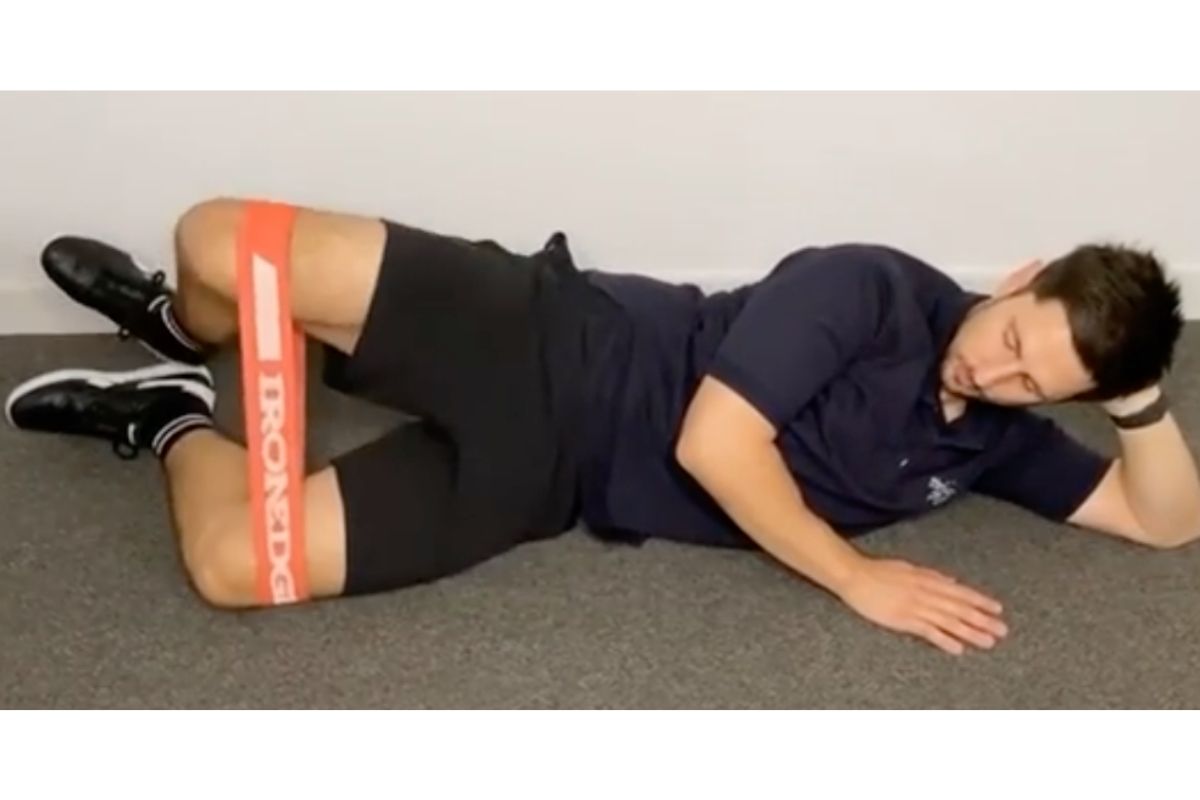
Some typical exercises that work for MOST people are pictured below. It should be noted that if any of these exercises increase your pain significantly or bring about severe pain you should stop immediately. However some mild discomfort when performing them is ok.







What are the symptoms?
- Mild to severe lower back pain, either focal to one point or can be diffuse across your lumbar spine below your ribcage
- On occasion, alongside back pain or discomfort you can get referred pain to the glutes, groin, front or back of your thigh and into the lower leg and foot.
- Combination of sharp pain with movement and aching pain at rest.
- You may feel increased stiffness or discomfort after sitting for long periods of time upon getting up
- Restricted range of motion
How to move when you have back pain
It is encouraged that you move as normally as you can, as moving in altered ways for weeks at a time can increase symptoms. Studies have shown that the simple act of walking regularly, within your pain limits can be helpful in reducing lower back pain.
In an acute episode, restricting the most painful movements for a short time only can be helpful to settle your symptoms in the early stages. However once severe pain has subsided, we will look to implement some full body movements within a few days to start the process of returning you to normal function and movement patterns.
This may involve some lower back mobility exercise and walking. As your pain and discomfort starts to decrease, performing exercises that challenge your trunk, core and legs form the basis of a robust lower back rehabilitation program.
Treatment plan & effective management
Early on, manual therapy treatment administered by an experienced physiotherapist which involves soft tissue massage, trigger point release or dry needling on your lower back and glutes for the first 2 weeks can help alleviate early discomfort and pain but also increase your confidence to move.
Alongside manual therapy, adding in strength exercises targeting the lower back, glutes and core muscles exercises as well mobility exercises focusing on lumbar spine range of motion are useful for reducing symptoms and starting the strengthening process.
As your pain settles, range of motion and confidence increases, the focus of treatment will shift away from hands on and will begin building your capacity to move through targeted lower body, core muscles strength and endurance exercise program.
What are the best exercises for lower back pain
A recent systematic review (A very high quality research paper) found that an exercise program with a combination of strength, flexibility and aerobic fitness exercise is beneficial for those with lower back pain (Gordon et al, 2016).
In an ideal scenario, a combination of these types of exercise should be incorporated into your exercise regime in order to help reduce recurrent back pain. However, doing something is better than nothing, so getting out for a walk a few times a week is better than nothing at all!
link to study.
Types of exercises for lower back pain include:
- Cobra press
- Open books
- Clamshells
- Planks
- Side planks
- Hip abduction with theraband
- Knee rocks
- Step ups
- Squats
- Lunges
- Lat pull downs
Side-effects of treatments:
Unlike some other treatments for low back pain like anti-inflammatory medication, cortisone injections and surgery, exercise and physiotherapy intervention has virtually no serious side effects. The only side effect you’re likely to have is to live a happier life with reduced pain and better function!
FAQs:
Is walking good for lower back pain?
Absolutely, it is one of the first things we will prescribe for those with low back pain. We recommend starting with 10-15 minutes in the morning and evening, but make sure it’s within your pain limits.
Are squats good for lower back pain?
Yes, once you’re feeling confident in your general movement, squats can be a great addition to your overall exercise routine.
How can you tell if back pain is muscular?
It can be difficult to determine this. Ultimately it doesn’t matter what specific structure is causing your pain, generally they are managed all the same and the prognosis is generally great!
Will massage help?
In the early stages of your recovery, absolutely but as your movement improves and pain decreases, best practice is to get you moving as soon as possible with appropriate exercise.
Should I get a scan?
Not right away! Your physiotherapist will rule out any red flags and ensure nothing severe or sinister is going on. We recommend chatting to your physiotherapist first, if needed your physio can refer directly for a scan . Give us a call on 8490 0777 or email us at [email protected] for personalised advice.
For more information about scans and lower back pain, see #4 in this post.

