Consider a skin callus. The hard, rough lumps we develop on areas of our body that are exposed to frequent, repetitive lifting, load and labour. Calluses are basically our body’s way of coping with this repetitive load in an effort to ‘harden up’ and allow us to continue doing what we’re doing- but without pain or further damage. Although not so sexy, they’re also not painful, and they’re there to serve a purpose.
Why are we discussing skin calluses? Because skin calluses are a great analogy for bursa sacs inside joints in the body.
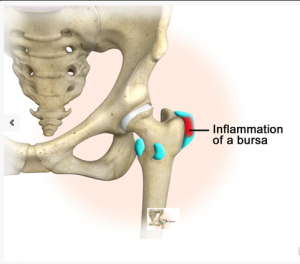

Bursa sacs are fluid-filled sacs that function as a gliding surface, reducing friction between tissues of the body. When bursa sacs become inflamed, it’s referred to as “bursitis”.
Thrive Physio Plus is conveniently located in Highgate at Shop 5/453 Fullarton Road. We provide expert physiotherapy services to the local Adelaide community, including residents of Malvern, Unley, Fullarton, and the 5063 area.
Bursitis is a diagnosis regularly thrown around by medical professionals, often seen in the conclusion paragraph of ultrasounds or other investigations from radiologists.
Essentially, bursa are just like skin calluses. They become irritated because it’s the body’s natural reaction to ‘harden up’ in response to increased amount of load at the joint, allowing the body to keep doing what we want it to.
People often have their bursae injected or even surgically removed in an attempt to reduce their pain and improve function. More often than not, a cortisone injection or other invasive interventions have very little effect. Why?
Clinically, we find that bursae are rarely the isolated cause of someone’s discomfort. Bursae become irritated because other structures in close proximity is causing it to become irritated.
Often we find by treating other structures around the joint, notably muscles and tendons with progressive strength work, we get significant relief from pain and improved function (including range of motion).
This leads to the burning question this blog post seeks to answer:
‘Is your pain and impaired function truly a result of an inflamed bursa or something else?’
Why Cortisone injections aren’t the answer
As therapists who treat ‘bursitis’ on a very regular basis, we find if we settle down the structures that are irritating the bursa, low and behold, we feel better and everything returns to normal.
Essentially, this is why after cortisone injections and other invasive interventions people still experience their symptoms. We are often not addressing what is the real driving factor behind their pain.
If you’ve been given the diagnosis of bursitis in your hip, shoulder or other joint but continue to experience pain and discomfort, we advise you seek a second opinion. It could be that your pain is, like a lot of other patients, not actually caused by an irritated bursa sac. You may be in need of gradual and progressive strength work to improve the capacity of that joint to deal with the work you’re asking of it.
If you or someone you know has experienced similar symptoms, call the clinic on 8490 0777 or book online here. One of our experienced physiotherapists can offer a thorough assessment to ensure you’re getting to the real root of your pain.
– The Thrive Physio Plus Team

